ABSTRACT
Joint hypermobility syndrome (JHS) and Ehlers-Danlos Syndrome (EDS) are both heritable disorders of connective tissue (HDCT) characterized by joint laxity and hypermobility. The conditions are both genetic disorders of collagen synthesis, where the adverse effects of tissue laxity and fragility can give rise to clinical consequences that resonate far beyond the confines of the musculoskeletal system. Both conditions have as their hallmark generalized hypermobility which can affect almost every bodily system. The hypermobility can be documented by the Brighton criteria which involves the objective measurement of the hyperextensibility of various joints. While the major presenting complaint of JHS and EDS is arthralgia in multiple joints, if the hypermobility is left unchecked, joint dislocations and degeneration may prevail.
While traditional medical treatments including education and lifestyle advice, behavior modification, physiotherapy, taping and bracing, exercise prescription, functional rehabilitation and pain medications offer some symptomatic control, they do little in regard to curbing the progressive debilitating nature of the diseases. The excessive joint mobility with its subsequent joint degeneration and multiple joint dislocations, can then lead the individual to seek out surgical intervention, which has suboptimal results in the hypermobile patient population versus the normal population. As such, some patients with JHS and EHS are seeking alternative treatments for their pain, including Prolotherapy.
Prolotherapy offers great hope for those with symptoms from generalized hypermobility because it is designed to successfully treat the ligament and tissue laxity that accompanies JHS and EDS. Prolotherapy works by initiating a brief inflammatory response, which causes a reparative cascade to generate new collagen and extra cellular matrix giving connective their strength and ability to handle strain and force. Prolotherapy has a long history of success treating ligament injuries, including patients with joint hypermobility. Studies on Prolotherapy have shown that it eliminates chronic pain even in those patients who have been told by their medical doctor(s) that surgery was the only treatment option for their pain.
Some of the rationale for using Prolotherapy for patients with EDS and JHS include that it has a high safety record, is comprehensive (all or most joints can be treated at each visit), is an outpatient procedure, is cost effective (compared to surgery), pain relief is often quick, and it provides joint stabilization. Perhaps its greatest asset is the fact that this one treatment modality can handle most of the painful musculoskeletal conditions that occur in individuals with EDS and JHS.
Prolotherapy could contribute to the treatment of hypermobility disorders also by preventing the development of precocious osteoarthritis. It has long been known that individuals with JHS and EDS suffer with premature osteoarthritis in various joints and the amount of degeneration correlates with the extent of the individuals hypermobility. The combination of extreme hypermobility and repeated injury is presumed to be what leads to the early osteoarthritis. This is most likely the reason that the hypermobility type of Ehlers-Danlos Syndrome is the most debilitating form with respect to musculoskeletal function.
While the primary author has twenty years experience treating JHS and EDS musculoskeletal symptoms with Prolotherapy, future studies will need to be conducted to best document the exact role Prolotherapy has in the treatment of the musculoskeletal symptoms and hypermobility of JHS and EDS and if it can prevent future joint degeneration in these individuals.
Journal of Prolotherapy. 2011;3(2):612-629.
EPIDEMIOLOGY
Joint Hypermobility Syndrome (JHS) is a largely under-recognized and poorly understood multi-systemic hereditary connective tissue disorder which manifests in a variety of different clinical presentations. Also termed heritable disorder of connective tissue (HDCT), this is a heterogeneous group of genetically determined diseases, with JHS being a milder variation of Ehlers-Danlos Syndrome (EDS), where gross joint laxity often prevails. While hypermobility is a feature common to them all, they are all believed to be caused by a defect in collagen, the essential connective tissue protein responsible for tensility and integrity of skin and joints tissues.1, 2
While Ehlers-Danlos Syndrome is the most severe form of hypermobility, many others suffer from similar conditions such as JHS, or even benign or undiagnosed forms of hypermobility, which present many of the same characteristics as EDS. Studies have indicated that JHS affects 2%–5% of the general population, although it is estimated that 1 in 20 hypermobile patients have not been diagnosed for their disorder.3, 4EDS is collectively believed to affect one in every 5000 children at time of birth, although this number is a rough estimate due to the fact that EDS is widely underdiagnosed in the general population.5, 6 At present, there are six primary known classifications of EDS: Classic, Hypermobility, Vascular, Kyphoscoliosis, Arthrochalasia, and Dermatosparaxis (See Figure 1.) The hypermobility type, which is found to be the most common, is estimated to affect one in every 10,000 to 15,000 individuals.7
| Classic | Hypermobility | Vascular | Kyphoscoliosis | Arthrochalasia | Dermatosparaxis |
|---|---|---|---|---|---|
|
|
|
|
|
|
ETIOLOGY AND PATHOLOGY
JHS has a strong genetic component with an autosomal dominant pattern. First-degree relatives with the disorder can be identified in as many as 50% of cases. Within this population, statistics indicate that EDS is more prevalent in those of African, Asian, and Middle Eastern descent, and affects women significantly more than men.8-10 The syndrome appears to be due to an abnormality in collagen or in the ratio of collagen subtypes. Mutations in the fibrillin gene have also been identified in families with JHS.11, 12
Ehlers-Danlos Syndrome is caused by defects in the biogenesis of collagen, the major structural protein of the body. The condition can be either inherited from a parent with the defect or caused by a genetic mutation. EDS is generally inherited in an autosomal dominant pattern, though an autosomal recessive type exists. Mutations in genes encoding fibrillar collagens or collagen-modifying enzymes have been identified in most forms of EDS, including the classic and vascular subtypes. To date, the genetic background of the hypermobility type of EDS remains unclear. The exact gene involved in hypermobility type EDS is unknown, although research indicates that there may be a connection to haploinsufficiency (having less than one half of the necessary amount) of tenascin X which is encoded by the gene TNXB.13Family history is an important tool in diagnosing EDS, because first-degree relatives have about a fifty percent chance of inheriting the defect.14 Unfortunately, there is no prenatal method of testing available to determine whether or not the defect has been passed down to a child.
When a defect such as the one found in EDS is present, collagen fibers become weakened, allowing tissues to become more elastic. In more severe cases, such as vascular type EDS, this can affect the tissues of the internal organs, such as the abdominal aorta, colon, and brain vessels, causing them to become weak and even rupture under pressure.15 In the case of JHS and hypermobility type EDS, the weakened collagen fibers affect the integrity of ligaments in the joints, and ultimately the stability of the joint. The weakness of these ligaments is what allows joints to hyperextend beyond the normal physiological limits.
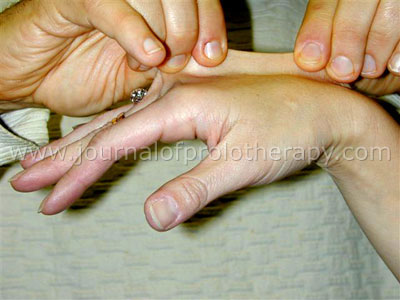
Joint hypermobility, a key finding in the heritable disorders of connective tissues, is diagnostically evaluated according to the Brighton Criteria, which utilizes the Beighton Score.** Determining the Beighton score is essential for making the diagnosis of JHS because it measures generalized joint laxity. The Beighton Score measures the ability to perform certain hyperextensive functions, including significant flexion of the thumb and fifth finger, hyperextension of both knees and elbows greater than 10 degrees, and the ability to place the palms on the floor with the knees fully extended, by assigning a point to each of these functions. (See Figure 2.) The Brighton criteria were developed to establish diagnostic criteria for JHS. Using these criteria helps physicians to distinguish JHS from other connective tissue disorders.16 According to the Brighton criteria, a score of four or higher on the Beighton Scale indicates generalized joint laxity and this along with athralgia in four or more joints for longer than three months signifies joint hypermobility syndrome.17,18 (See Figure 3.) Typically a score of five or higher on the Beighton Scale is used as the cut-off for Ehlers-Danlos Syndrome.**

| Brighton Criteria |
|---|
Major Criteria
Minor Criteria
Requirements for Diagnosis
|
**There is still some debate on the necessary criteria for making the diagnosis of Ehlers-Danlos Syndrome (EDS). While a Beighton score of 5 is indicative of EDS, a score of 4 does not preclude the diagnosis. Most agree that the diagnosis is made by a family history of the condition and the clinical evaluation. Genetic testing and muscle and skin biopsies confirm the connective tissue (collagen) disorder. Other diagnostic testing such as echocardiogram, MRIs and CT scans can be used to confirm blood vessel, valvular, and organ connective tissue problems seen in the various types of EDS.
CLINICAL PRESENTATION
While joint hypermobility is very common, occurring in 10-20% of populations of Western countries, and higher still in those in Indian, Chinese, and Middle Eastern groups, it is important to distinguish between joint hypermobility and Joint Hypermobility Syndrome.19 People who are hypermobile without symptoms are merely people with hypermobility. Those with symptoms attributable to their hypermobility may have JHS if they conform to the Brighton criteria.
While hypermobility with arthralgias (joint pain), may sound rather benign, JHS is typically a multi-system disease that can be quite disabling. In one study out of the University of Manchester involving 125 children with JHS, 74% had arthralgia, 13% speech difficulties, 14% learning difficulties, 12% urinary tract infections 10% subluxation/dislocations of joints, while 48% had limitations of school-based physical education activities, and 67% difficulties in other physical activities.20 Because of deconditioning, children with JHS have been found to have a significantly decreased maximal exercise capacity compared with age and gender-matched control subjects.21 Another study linked an increased prevalence of migraine headaches with JHS.22 It is not uncommon for patients with JHS to go 10 years or more before getting appropriately diagnosed.23 One reason for this is doctors and others are trained to examine for reduction of joint mobility rather than for an increased range, so that hypermobility is commonly missed. When hypermobility is sought it is the most common finding among patients presenting to a rheumatologist, but more often than not, is overlooked.24 Nearly one-half of rheumatologists are skeptical about the significant impact that JHS has on people’s lives, and about three-quarters are skeptical about a significant contribution to the overall burden of rheumatic diseases.25 Besides arthralgias, generalized joint laxity, the hallmark of the HDCTs, including JHS, is a significant risk factor for conditions such as joint dislocations, temporomandibular disorders, pathologic disc degeneration, diffuse idiopathic skeletal hyperostosis, osteoarthritis, as well as joint injury during sports.26-30
Typical clinical manifestations of JHS and EDS are abnormalities of the skin, joint hypermobility, recurring joint dislocations, and arthralgia. Skin abnormalities can include thin, transparent skin, significant skin hyperelasticity, easy bruising, poor wound healing, and atrophic “cigarette paper” scars. Joint symptoms, which represent some of the more severe aspects of these conditions, range widely; however, the most frequent complaints are joint pain and dislocations. Patients with JHS often say that they are “double jointed” or that they can contort their bodies into strange shapes (i.e. voluntary subluxations) or do the splits. Many JHS patients have signs and symptoms suggestive of fibromyalgia and are usually misdiagnosed.31 These patients present with a wide variety of readily identifiable traumatic and overuse lesions, such as traction injuries at tendon or ligament insertions, chondromalacia patella, rotator cuff lesions, or back pain due to soft tissue injury or disc herniation. Others suffer the effects of joint instability, such as flat feet, recurrent dislocation or subluxation-notably of the shoulder, patella, metacarpophlangela joints, or temporomandibular joints. Others still, develop a chronic degenerative arthritis that may be a direct complication of JHS (See Figure 4.) For those who suffer from dislocation of joints, the pain can be immense, and sometimes is the first indication a patient has hypermobile joints. Many hypermobile patients also experience myofascial pain, which may be explained by the extra stress placed on muscles to compensate for lax joints as the muscles attempt to stabilize the joints.
| Example: A shoulder, knee, or elbow is lax or prone to dislocation.Ligament laxity occurs in a single joint or multiple joints independent of each other. Only symptoms are hyperextension and arthralgia.Beighton score: 1-3 |
Example: Joint Hypermobility SyndromeHypermobility of four or more joints occurs in the absence of any rheumatologic disease. Characterized by joint hyperextension, arthralgia, and joint dislocation or vertebral subluxation.Beighton score: >4Brighton criteria: 2 Major Criteria or 1 Major and 2 Minor Criteria, or 4 Minor Criteria |
Example: Ehlers-Danlos Syndrome, Hypermobility Type Marfan Syndrome Osteogenesis ImperfectaHypermobility is congenital and caused by an inheritable defect. Effects are multisystemic and can include cardiac, optical, uterine, gastrointestinal, respiratory, spinal, integumentary, and joint abnormalities.Beigton score: >5Brighton criteria: 2 Major Criteria, 1 Major and 2 Minor Criteria, or 4 Minor Criteria |
One of the more serious long-lasting affects of joint laxity is chronic joint degeneration. The increased mechanical stress caused by ligament laxity leads to chronic joint instability, making them more susceptible to soft tissue injuries. Continual instability and injury leads to an earlier onset of degenerative joint disease in hypermobile and other patients with ligament injuries than in the normal population.32-34
While the signs of a typical HDCT may be present, including scoliosis, pes planus, genu valgu, lordosis, patellar subluxatin or dislocation, marfanoid habitus, varicose veins, rectal or uterine prolapsed, or thin skin, often the only manifestation are hypermobile joints. Because young children are generally very flexible, the presence of a hypermobility disorder can go undiagnosed for years; joint symptoms often will not surface until adolescence as the patient becomes more active and prone to dislocation and injury.
There is an urgent need to increase the awareness of JHS and spectrum of HDCTs. These are prevalent conditions that are frequently undiagnosed and that can cause significant health problems. Beside recurrent musculoskeletal problems and signs and symptoms derived from tissue fragility, adolescents and young adults may develop osteoporosis, early osteoarthritis or dysautonomia, that are common in the disease and deteriorate quality of life. Doctors may be unaware of the prevalence of the condition, its effect on quality of life or its multisystemic nature, and may not routinely look for hypermobility in the clinical examination, especially as the condition rarely forms part of the curriculum in medical schools or in postgraduate training programs.35-37
The erroneous view that hypermobility is a variant of normality, rather than part of an inherited connective tissue disorder is still widely held. If joint hypermobility syndrome and the other inherited connective diseases are missed on a physical examination the following problems may arise:
- Inappropriate and potentially harmful labeling or treatments may be applied on the basis of an erroneous diagnosis such as fibromyalgia, degenerative disc disease, hypochondriasis, or degenerative arthritis.
- Overzealous physical manipulation which make hypermobile joints even more lax.
- Orthopaedic operations may be done without the surgeon knowing the patient has an underlying connective tissue disorder, which may lead to poor outcomes.
- Chronic pain may lead to a potentially reversible downward spiral of immobility, deconditioning, dependency, and despair. Out of 700 patients with JHS attending the UCH Hypermobility clinic, 168 were experiencing serious pain, disability and impairment of their quality of life, some patients becoming chairbound or even bedbound.38
While hypermobility may be generalized or extreme in a small number of joints, it is important for pain physicians to recognize when it is present. Besides knowing the Brighton criteria, based on determination for the Beighton Score, comparing a patient’s joint range of motion compared with normal ranges for age and sex can give a clinician a clue that joint hypermobility is present. There are other common clues in both children, adolescents and adults that suggest Joint Hypermobility Syndrome is present. Some of the clues that a patient has joint hypermobility include: recurrent joint dislocations, frequent ankle sprains, child with poor ball catching and handwriting skills, premature osteoarthritis, as well as laxity in other supporting tissues. (See Figure 5.) A small proportion of patients with generalized joint hypermobility will have one of the more serious conditions such as Ehlers-Danlos Syndrome, Marfan Syndrome or Osteogenesis Imperfecta. When these more serious conditions are considered, a referral is made to a geneticist or other clinician for genetic testing, skin biopsy or diagnostic tests, such as an echocardiogram to look for valvular defects, or other diagnostic tests on other organs to search for signs of a multisystem connective tissue disorder. It is important to differentiate JHS from the Vascular Ehlers-Danlos Syndrome, for instance, to prevent life threatening vascular hemorrhages from arterial ruptures in the latter condition.
In children and adolescents*
In adults
|
DIFFERENTIATING EHLERS-DANLOS SYNDROME FROM JOINT HYPERMOBILITY SYNDROME
Ehlers-Danlos Syndrome should be considered in the evaluation of every hypermobile patient who has a pain complaint. A key characteristic for diagnosis and differentiation of EDS from JHS is the addition of skin findings.39 EDS type 1 and type 2, previously known as EDS classic type, has skin that extends easily and snaps back after release. (See Figure 6.) The skin is fragile, as manifested by splitting of the dermis following relatively minor trauma, especially over pressure points (knees, elbows) and areas prone to trauma (shins, forehead, chin). Wound healing is delayed, and the stretching of scars after apparently successful primary wound healing is characteristic. While EDS type 4, vascular type, can have all of the above, besides easy bruising and hematoma formation in areas of trauma, the skin is translucent (visible veins on the chest).40 These skin findings are in contrast to EDS type 3, hypermobility type, which has soft skin with normal or only slightly increased extensibility.41
All forms of EDS, like JHS, affect the joints, causing hypermobility, and as a result, individuals are more susceptible to dislocations, subluxations, sprains, strains, and sometimes fractures. While there is no distinguishing feature of the joint and neuromuscular symptoms of EDS versus JHS, EDS is often more disabling.42, 43 The results of one study showed that 1) chronic pain in EDS is highly prevalent and associated with regular use of analgesics; 2) pain is more prevalent and more severe in the hypermobility type; 3) pain severity is correlated with hypermobility, dislocations, and previous surgery; 4) pain is correlated with low nocturnal sleep quality; and 5) pain contributes to functional impairment in daily life, independent of the level of fatigue. The authors concluded, “Therefore, treatment of pain should be a prominent aspect of symptomatic management of EDS.”44 In another comprehensive study on EDS, researchers found that over 90% suffered with chronic pain; eight was the mean number of pain locations; 70% reported continuous pain in their lower extremities, ankles, feet, toes, and hips; 89% of the pain began in childhood or adolescence; 88% were or had taken pain medications; and 51% needed narcotics. These authors concluded, “In summary, our data reveals that individuals with EDS experience frequent and severe pain through much of their lives.”45 The severe crippling pain of EDS often prevents patients from participating in sports and having a lower quality of life.46 Other authors have confirmed the widespread pain symptoms of the condition with the hypermobility type of EDS to be the most debilitating form, with respect to musculoskeletal function, especially affecting ambulatory ability.47, 48
TRADITIONAL TREATMENTS
Management of JHS and EDS frequently includes education and lifestyle advice, behavior modification, manual therapy, taping and bracing, electrotherapy, exercise prescription, functional rehabilitation and collaborative working with a range of medical, health and fitness professionals.49 Progress is often slow and hampered by physical and emotional setbacks. The functional rehabilitation process is frequently lengthy, with education of the patient and family, sensitively prescribed and monitored physical therapy interventions and facilitation of lifestyle and behavior modifications being the mainstay of the plan.50Sometimes with a carefully considered management strategy, amelioration of symptoms and independent functional fitness can sometimes be achieved. Currently, there are no randomized controlled studies regarding the effects of existing treatments.51
At present, there is no cure for collagen and connective tissue deficiencies of Joint Hypermobility Syndrome and Ehlers-Danlos Syndrome. The musculoskeletal symptoms derive from a vulnerability to injury resulting from fragile collagenous tissues (tendon, ligament, muscle, bone, cartilage, menisci, labrum, and skin). Conservative treatments such as physiotherapy can help hypermobile patients by the use of mobilizing techniques to restore subluxations; enhance general fitness to offset or reverse the tendency for the body to lose condition by lack of exercise; core and joint stabilizing and proprioception enhancing exercises to decrease pain and prevent further injuries.52 As joint complaints increase with vigorous and repetitive activities, patients with JHS and EDS learn that overtraining and exercises that focus on joint flexibility rather than stabilization increase joint pain and risk of injury, thus, they need to be curbed.53, 54 Patients refrain from activities that cause joints to lock or overextend. If avoidance of these activities is not an acceptable option for patients, physicians often try other approaches including chiropractic or osteopathic manipulation. While these approaches can give some symptomatic relief they offer little as far as long term solutions.55, 56
Pain management is a critical element in the treatment of hypermobility. While physical therapy and exercise may lend some degree of pain relief, individuals with hypermobility often require additional measures to manage joint pain. Patients with hypermobility disorders are often prescribed large doses of pain medication, such as acetaminophen, muscle relaxants, NSAIDs, and antidepressants; over time, stronger medications (including narcotics) and higher doses may be required to deal with the effects of chronic pain. These medications are helpful in management of symptoms that prohibit patients from carrying out certain activities, but they have no effect in treating the underlying pathology of hypermobility, and in some cases they may actually have a negative effect on joint tissues. Non-steroidal anti-inflammatory drugs (NSAIDs) are one class of medications commonly prescribed for joint pain, but can have a combative effect on joint health, due to their role in inhibiting the synthesis of collagen and articular cartilage synthesis.57 This can cause not only weakness in ligaments, but also in cartilage, tendon, and bone cells, contributing to an overall weakening of the joint.58, 59
Another approach used to help with the painful symptoms of hypermobility is splinting and bracing to try to stabilize the joints. This, along with proper physical and occupational therapy to help strengthen muscles and to educate people how to properly use and preserve joints is helpful, but limited. In general, traditional medical intervention is limited to symptomatic therapy. When the symptoms continue to progress and/or are of an emergent or severe nature then surgical intervention is called upon.
Many individuals will have undergone several orthopedic procedures, even prior to diagnosis. It is quite common for the average patient with EDS, or those severely affected with JHS, to undergo multiple musculoskeletal surgeries throughout their lifetime to combat joint injury degeneration and dislocations from hypermobility.60 Common operations include tendon transplant or transfer, capsulorraphy, arthroscopic surgery and arthroplasty.61, 62 The degree of stabilization and pain reduction, overall patient satisfaction, and duration of improvement are quite variable. Unfortunately, the weakness of hyperelastic joint tissue presents a poor healing prognosis, and surgery has proven to be widely unsuccessful in the hypermobile population.63, 64 Grahame and Keer explain that this is because hyperelastic tissues are “less robust and amenable to surgical procedures” than healthy joint tissues.65When surgery is performed, the patient and physician should cautiously anticipate some improvement but expect less than optimal results.66 While such surgical measures may provide temporary pain relief and stabilize the joint for a short time, using the surgical treatment model for cases of severe generalized hypermobility poses a problem on account of the following:
Capsulorraphy – suture of a tear in a capsule, especially of a joint capsule to prevent recurring dislocation.
Arthroscopy – examination of a joint, specifically, the inside structures and then repair or remove damaged structures.
Arthroplasty – surgery to relieve pain and restore range of motion by realigning or reconstructing a joint.
- The underlying systemic connective tissue deficiency makes surgical outcomes less predictable.
- The condition is systemic and involves multiple joints and body tissues.
- The amount of surgical procedures can be unending because of the systemic nature of the conditions.
- Each subsequent surgical procedure on any given tissue or joint is less successful.
The lack of long-lasting relief in any of these traditional treatments provides a grim prognosis for anyone living with the chronic disabling pain of Joint Hypermobility Syndrome and Ehlers-Danlos Syndrome. The common flaw in each of these traditional treatments is their inability to repair the weakened connective tissues causing the hypermobility. Logically, then the best approach would be the one that directly addresses the root of the disability, weakened connective tissues, such as ligaments and joint capsules, by inducing their repair to stabilize the affected joints.
PROLOTHERAPY
Because surgery carries risks and complications and often does not cure pain symptoms in patients with JHS and EDS, patients are seeking alternatives with the same or greater results. Prolotherapy is one alternative that patients are turning to. Prolotherapy works by initiating a brief inflammatory response, which causes a reparative cascade to generate new collagen and extra cellular matrix giving connective tissue their strength and ability to handle strain and force.67, 68 High-resolution ultrasounds and MRIs have been used to confirm that Prolotherapy does indeed stimulate tissue growth.69, 70 One double-blinded animal study by Dr. Liu showed that Prolotherapy increased ligament mass by 44%, ligament thickness by 27%, and ligament bone junction structure by 28%.71 A human double-blinded study showed joint stabilization by Prolotherapy correlated with patient outcome improvement.72
The doctor that introduced Prolotherapy into mainstream medical practice was George S. Hackett, MD, who described it as follows, “The treatment consists of the injection of a solution within the relaxed ligament and tendon which will stimulate the production of new fibrous tissue and bone cells that will strengthen the weld of fibrous tissue and bone to stabilize the articulation (where the bone and ligament meet) and permanently eliminate the disability.”73 He published his results in peer-reviewed, mainstream medical journals and wrote a book summarizing his results and the technique entitledLigament and Tendon Relaxation Treatment by Prolotherapy.74-76 He showed via animal studies that Prolotherapy induced the proliferation of new ligament tissue that had the effect of stabilizing joints, thereby eliminating the disability associated with ligament laxity.77-79
Prolotherapy has a long history of success treating ligament injuries, including patients with joint hypermobility.80, 81 Studies on Prolotherapy have shown that it eliminates chronic pain even in those patients who have been told by their medical doctor(s) that surgery was the only treatment option for their pain.82-85 Some of the rationale for using Prolotherapy for patients with EDS and JHS are that it has a high safety record, is comprehensive (all or most joints can be treated at each visit), is an outpatient procedure, is cost effective (compared to surgery), pain relief is often quick, and it provides joint stabilization. Perhaps its greatest asset is the fact that this one treatment modality can handle most of the painful musculoskeletal conditions that occur in individuals with EDS and JHS. (See Figure 7.)
| List of Musculoskeletal Conditions |
|---|
|
Prolotherapy could also contribute to the treatment of hypermobility disorders by preventing the development of precocious osteoarthritis. It has long been known that individuals with JHS and EDS suffer with premature osteoarthritis in various joints and the amount of degeneration correlates with the extent of the individuals hypermobility.86-88 Dr. P. Brighton who developed the criteria to determine joint hypermobility (for whom the Brighton criteria is named) found that when individuals had Ehlers-Danlos Syndrome and a Beighton score of at least 4, 100% of them developed osteoarthritis by the age of 40.88 The combination of extreme hypermobility and repeated injury is presumed to be what leads to the early osteoarthritis. This is most likely the reason that the hypermobility type of Ehlers-Danlos Syndrome is the most debilitating form with respect to musculoskeletal function.89
TWENTY YEARS EXPERIENCE TREATING JOINT HYPERMOBILITY SYNDROME AND EHLERS-DANLOS SYNDROME WITH PROLOTHERAPY
I (R.H.) joined the practice Gustav A. Hemwall, MD in 1993, at which time Dr. Hemwall had already been performing Prolotherapy for nearly 40 years after learning the technique from Dr. George Hackett at his office in Canton, Ohio in the mid 1950s. I can remember the point Dr. Hemwall made to me in April of 1992, while first observing in his office. He said, “Most chronic pain is from ligament laxity.” When I finished my first draft of Prolo Your Pain Away! there was a small section on both benign congenital hypermobility (also termed Joint Hypermobility Syndrome) and Ehlers-Danlos Syndrome. The reason for including them was obvious. Prolotherapy caused a significant improvement in the quality of life of individuals who had a genetic connective tissue disorder causing systemic hypermobility, the very condition (though extreme) for which Hackett-Hemwall Prolotherapy was designed to treat. One patient in those early years of working with Dr. Hemwall comes to mind.
JM was a young woman in her 30’s, who had the hypermobility type of EDS, and was already confined to a wheelchair when she originally consulted with Dr. Hemwall. By the time I first saw her, she was walking, running and leading a normal and fulfilling life. Initially, she required intensive Prolotherapy for about 18 months, then twice a year for a couple of years. But after that time she was done with treatment. Prolotherapy had stabilized the joints enough, to where now it has been over 10 years since she required treatment. The intensive Prolotherapy involved treating most of the joints in her body, and she was treated over the course of two days each time. The first day, she would receive treatment to half of her joints, and the second day the other half would be treated. This is an extreme case, but mentioned to show the extent of the possibilities with Prolotherapy.
REPRESENTATIVE CASE HISTORY
JD presented to Caring Medical with a long history of severe joint pain and complaints of frequent dislocations of both elbows, knees, and shoulders, as well as subluxations throughout the spine and the sacroiliac (SI) joints. She had first begun experiencing joint pain at the age of ten, and her symptoms escalated during her teen years as she became an avid track and field athlete. The first incident of joint dislocation occurred when her knee completely gave out during a track meet. Following this event, JD underwent multiple knee reconstructive surgeries which provided short term relief, but she continued to experience pain and instability in that knee. At the age of 21, JD began experiencing cardiovascular symptoms including tachycardia and feeling faint. When she consulted a cardiologist, JD learned that she suffered from Ehlers-Danlos Syndrome.
Over the course of her adult years, JD’s condition began to affect other joints in her body including her shoulders, elbows, and sacroiliac joint. Simple activities such as walking, or even a strong wind, JD said, could cause her joints to dislocate on a daily basis. In addition to being unable to walk, she was unable to use crutches or a cane because these would cause dislocation in her shoulders and elbows. Like many others who suffer from Ehlers-Danlos Syndrome, JD’s condition had impeded her education and prohibited her from being able to work for extended periods at a time. When she came to Caring Medical for evaluation, JD had already undergone eight unsuccessful musculoskeletal surgeries and years of physical therapy, with no lasting improvement. Unless she found an effective treatment for her condition, she would be disabled for the rest of her life. Her initial questions were simple: Could Prolotherapy prevent the multiple joint dislocations that were occurring on a weekly basis? Could Prolotherapy give her enough pain relief so she would not be disabled the rest of her life and be strong enough to find work and support herself? The answer, based on my experience (R.H.) with treating Joint Hypermobility Syndrome and Ehlers-Danlos Syndrome to both questions is a solid “yes.” However, it should be noted that if an individual with JHS or EDS is treated early in the disease course, where hypermobility is their primary problem, the extent of the Hackett-Hemwall Prolotherapy needed will be much less than after the person has suffered from multiple dislocations and several reconstructive joint surgeries.
CASE STUDIES
Caring Medical is a comprehensive Prolotherapy practice. In the years 2009-2010, 102 patients were seen, with 85 being women and 17 being men, who carried the diagnosis of Ehlers-Danlos Syndrome or Joint Hypermobility Syndrome. This represented approximately 8% of the total patients seen during this time. The following cases are typical of the response one would expect utilizing Prolotherapy in the treatment of JHS or EDS, where resolution of the individual’s joint instability/hypermobility is the primary concern.
CASE STUDY: 21 YEAR-OLD FEMALE WITH EHLERS-DANLOS SYNDROME, HYPERMOBILITY TYPE
EK first began experiencing the symptoms of Ehlers-Danlos Syndrome, Hypermobility type in the fifth grade, when one of her knees subluxed. Over the next 12 years, the pain and joint subluxations spread to other joints including the other knee, elbows, shoulders, and spine. EK tried many different forms of therapy including physical therapy, massage, ultrasound, taping, and compression braces which managed her pain well enough to perform daily activities as well as gymnastics, track, and cross country. At the age of 19, she tore the meniscus in her right knee and underwent surgical meniscus repair. Following the operation, she experienced intense pain, and subsequently underwent a second operation. While the symptoms in her knee appeared to be resolved, pain in her other joints persisted. During this time, EK also began experiencing other health issues including hypothyroidism, eczema, chest pains, food allergies, irregular menstrual periods, and degenerative disc pain in her neck and back.
In the search for a treatment for her joint pain, EK found Prolotherapy, which she felt was needed for the pain in her neck, thoracic, low back, knees, and shoulders. During this time, she continued physical therapy, and managed her pain with multiple medications. After a year and a half of minimal improvement, her pain doctor referred her to Caring Medical in Oak Park, Illinois for Prolotherapy. As a 21 year-old college student, EK was living with constant joint pain, which disturbed her ability to exercise, study, and sleep. She contemplated dropping out of school. By this time, she also suffered from joint dislocations in her shoulders and elbows causing its own amount of excessive pain and stiffness. Her spine, including the neck, thoracic, and lumbar regions, would also “freeze,” sending shooting pain up and down her back.
EK’s first Prolotherapy treatment at Caring Medical consisted of Prolotherapy injections to her neck, spine, both scapulas, low back, and knee. Within a week of her first visit, EK reported a decrease in her thoracic and scapular pain and improved physical stamina and energy. A month later, she began running again and no longer required treatment to her knee. By her second visit, EK had discontinued all use of pain patches, and only required occasional Tylenol for pain and muscle relaxers to help her sleep. For the next six months, EK continued to receive monthly treatments to her neck, thoracic, and shoulders, showing gradual improvement of pain and well-being. After eight months of treatments, EK no longer required any pain medications, was no longer experiencing any joint dislocations, and was back to running and gymnastics. After her initial eight months of therapy, she was seen an average of once per year throughout her college and Masters program. She has not been seen for treatment for over seven years now, during which time she has received a PhD in her chosen profession. She continues to lead a full life, without daily pain or disability. She has no limitations while exercising most days.
DISCUSSION:
Sometimes Prolotherapy is so successful that when the joints are stabilized, even clients with Ehlers-Danlos Syndrome, do not need further treatments. To be fair, EK did need more than the customary three to six visits, most likely because of the Ehlers-Danlos Syndrome. I have not seen this client for over seven years, but have communicated with her, and I can emphatically say that she now has a completely normal productive life. She went from living in fear of multiple subluxations in multiple joints, to complete stability in those joints, even with exercising most days. Prolotherapy, in this patient with Ehlers-Danlos Syndrome, appears to have permanently stabilized the unstable joints. The next case is presented because some patients with Ehlers-Danlos Syndrome, Hypermobility type, need periodic care to keep the various joints from dislocating or subluxing.
CASE STUDY: FEMALE WITH EHLERS-DANLOS SYNDROME, HYPERMOBILITY TYPE
PF is now a 55 year-old retired school teacher and mother of two adult children who lives in Canada. She came to Caring Medical because her Prolotherapy doctor, Fred Cenaiko, MD, retired. She had always known she was “hyperflexible” but had controlled her various joint aches, pains, and subluxations with physiotherapy and chiropractic care. Her pain became unbearable 15 years prior to the first visit at Caring Medical, when she began experiencing pain and instability in her left sacroiliac (SI) joint. After seeing many specialists over the course of several months for her SI pain, including her general practitioner, orthopedists, physiotherapists, and chiropractors, PF was left upset and disappointed by her continued pain and lack of improvement. She was having difficulty working, in addition to raising her two children. If something wasn’t found to help the unrelenting pain, she was destined to soon be completely disabled. Chiropractic adjustments helped for a few hours only to have her lower back go out again. She was told by one orthopedist to get a sacroiliac fusion.
As her low back pain increased, so did the rest of her joint pain. Her popping, clicking, and a feeling of looseness throughout her body increased. No longer were physiotherapy and chiropractic manipulation able to control her pain. Within a year, she had whole body pain and instability that almost completely disabled her for two and a half years. She was unable to take care of her children and she had to rely on strong pain medications in order to function. One day, her European-trained physiotherapist gave her some research articles from medical journals that talked about the tightening of joints with Prolotherapy. PF noted that the main doctor doing Prolotherapy was in Oak Park, Illinois, Dr. Gustav Hemwall. When she called Dr. Hemwall’s office, she was referred to Dr. Fred Cenaiko who worked in Saskatchewan, Canada. It was Dr. Cenaiko who diagnosed PF with Ehlers-Danlos Syndrome, Hypermobility type, and began treating her back and other areas of her body every six weeks with Hackett-Hemwall dextrose Prolotherapy. It took PF, 1.5 years of receiving dextrose Prolotherapy to her lower back to experience complete resolution of her SI pain. She reports that her other joints, including her knees, shoulders and hips healed much more quickly and she only required a couple treatments to each joint to resolve her pain complaints.
After one and a half years of doing Prolotherapy, PF was completely pain free. Because various joints of her body would begin to sublux and become painful over time again, she and Dr. Cenaiko realized that receiving Prolotherapy two to three times a year was what was needed to keep her stable and pain-free. PF has continued to receive Prolotherapy two to three times per year for the past 13 years. She was able to complete the necessary years as a teacher to be eligible for full retirement benefits from teaching. Prolotherapy also helped her get back to being the type of mother, wife, and friend that she wanted to be. PF currently swims laps, jogs, or hikes on a daily basis with no pain. She states that she also enjoys biking but she has to be careful because if she cycles at a high resistance for long distances, her knees start to become unstable. PF also avoids massages because she has noticed that massages tend to loosen her joints. Dr. Cenaiko retired in 2010 and referred PF to Caring Medical to continue her maintenance Prolotherapy treatments.
DISCUSSION:
It has not been the “norm” at Caring Medical for a client with Ehlers-Danlos Syndrome to need periodic Prolotherapy treatments. Dr. Cenaiko used dextrose as the proliferant for PF. When I evaluated her and noticed that indeed there were some joints that were unstable, I suggested at her first visit to Caring Medical that we use a strong proliferant. To start, she received dextrose Prolotherapy with sodium morrhuate added to the solution. While she still believes she will need Prolotherapy twice per year, it is my hope that we will get her joints stable enough with the stronger Prolotherapy treatments, that eventually she will no longer need Prolotherapy.
This case is presented here so patients with Ehlers-Danlos Syndrome know that generally Prolotherapy can permanently stabilize joints. But some patients, like PF, are happy that Prolotherapy is available if periodic treatments are necessary.
CASE STUDY: 31 YEAR-OLD FEMALE WITH JHS, WITH CONSTANT SHOULDER, THORACIC AND RIB SUBLUXATIONS
NP is a 31 year-old registered dietitian who came to Caring Medical in February 2009 from a referral by her osteopathic doctor, because of the diminishing benefits manipulation was having on her pain. She was very interested in the potential benefits Prolotherapy might have on her significant shoulder and thoracic/rib pain. She stated that she “has always had loose joints” and for most of her adult life has needed either chiropractic or osteopathic care to function. Her significant pain started 10 years earlier while on the rowing team at college. Her primary pain was located in the left T1-T4 area and left shoulder. A previous MRI of the thoracic area was read as normal. She had tried acupuncture, electrical stimulation, physical therapy, and various medications and manual therapies without lasting relief.
On physical examination, she had noticeable ligament laxity in multiple thoracic/rib junctions (costovertebral) and her left shoulder easily subluxed anteriorly. Her Beighton Hypermobility Score was 5. At the initial visit, dextrose Prolotherapy was given to her left thoracic facets and costovertebral junctions. When seen one month later, she felt 40% better and another Prolotherapy treatment was given to the same area. She was not seen again until June and felt her thoracic pain didn’t need treatment anymore but she wanted to start treatment for her left shoulder instability. Because of the degree of instability, sodium morrhuate (1cc/10cc syringe) was added to the dextrose Prolotherapy solution and treatment was given primarily to the anterior shoulder.
NP did not return for one year because of resolution of her thoracic and shoulder pain with the previous Prolotherapy treatments. When seen in June 2010, her primarily complaints were clicking, pain and an “unstable feeling” in the left hip. On physical exam, a definite palpable click was felt and a moderate degree of instability was seen. Her anterior and posterior left hip was treated on that date and again one month later. She had complete resolution of these symptoms. She was seen in October 2010 because of low back pain which wasn’t resolving with physical therapy and exercises. Physical examination revealed hypermobility of her left sacroiliac joint. Dextrose Prolotherapy with sodium morrhuate was administered to the left lower back region emphasizing treatment of the left sacroiliac joint.
When NP was seen again in February 2011, the only complaint she had was recurring subluxation of her left shoulder joint during activity. She again had evidence of shoulder joint instability anteriorly. Treatment of dextrose Prolotherapy with sodium morrhuate to this area resolved this issue.
DISCUSSION:
It is common with genetic hypermobility cases for symptoms to “pop” up in other joints once the primary painful and hypermobile areas are stabilized with Prolotherapy. For instance, NP had hip instability that was stabilized with Prolotherapy, subsequently causing her hypermobile left sacroiliac joint to cause symptoms. The nice effect of Prolotherapy is that even with genetic hypermobility syndromes, the joint pain is often relieved permanently. But sometimes periodic treatments are needed because of the recurrence of joint hypermobility in a previously treated area.
CASE STUDY: 22 YEAR-OLD COLLEGE STUDENT, SELF-MANIPULATOR WITH SEVERE BILATERAL SHOULDER AND KNEE PAIN AND INSTABILITY
JR, a 22 year-old male college student, came to Caring Medical in April of 2010 for complaints of bilateral knee swelling and shoulder instability. His lateral knee swelling began after he took up running in 2009 in preparation for entering the military upon graduation from college. He stopped running and was evaluated by an orthopedic surgeon who did an MRI and found an oblique tear of his lateral meniscus in both knees. The surgeon recommended arthroscopic surgery but JR looked for an alternative. He received one platelet rich plasma (PRP) injection on three separate visits with only minimal help. He sought a consultation at Caring Medical for Prolotherapy because of the minimal improvement with the PRP injections alone.
His shoulder issues started in 2005 (at age 17) after he tore the labrum in his right shoulder and had surgery to repair the tear. Despite having surgery, he continued to feel instability and pain in his shoulder. Because of his bilateral knee and shoulder pain and instability, even his ability to do non-impact sports like swimming had been affected.
Physical examination revealed joint hypermobility throughout his body, with a Beighton Hypermobility Score of 5. JR admitted that he frequently self adjusts or pops many of the joints in his body. Physical examination of his knees revealed significant bilateral grinding/crepitation with moderate to severe patellar hypermobility. He was instructed not to self manipulate his joints upon starting Prolotherapy, as this could potentially disrupt the connective tissues that are repairing after treatment. Dextrose Prolotherapy with sodium morrhuate was administered around the patella, as well as the various ligaments of both knees. Bilateral intraarticular Human Growth Hormone (2iu/joint) was also given. Because of the improvement in his knee pain with the first treatment, when seen one month later, his shoulders were also treated. He did not return until five months later, because of some continued symptoms, though he was feeling more stability and strength in his knees and shoulders. The knees were no longer swelling and he was back to an active exercise program.
JR returned for three more treatments from October to December 2010. This totaled five treatments to his knees and three treatments to his shoulders. At his last visit, JR reported that he was back to swimming and weight training without limitation, and only had an occasional crepitation in his shoulders but did not have pain. As for his knees, the crepitation was greatly decreased as well as the swelling. He has not yet tested his knees by running.
DISCUSSION:
This case shows that some folks, even with Joint Hypermobility Syndrome, may be doing something to themselves to worsen his or her condition. In this case, JR was what we term a “self-manipulator.” He was manipulating himself an estimated hundred times per day. It becomes a habit. He cracks his neck, low back, thoracic, shoulders and other joints. It is imperative for hypermobile patients not to self-manipulate as this just further stretches the ligaments and makes them even more hypermobile. Eventually they are so loose that the only way they can keep in place to is to self manipulate. Obviously, Prolotherapy to the joint and spine instabilities is a better option. In JR’s case, I (R.H.) believe he should get treated until he is back to running.
CASE STUDY: 18 YEAR-OLD FEMALE GOES FROM ANTI-DEPRESSANTS AND ANTI-ANXIETY MEDICATIONS TO PAIN FREE AT 28
When SB came to Caring Medical in March 2009, you would not have believed that this was the same woman who had walked into the office in 2001 as an 18 year-old. She was now a graduate of the prestigious Chicago Art Institute, happily married, and able to exercise. She was taking no medications. This was a far cry to the person seen in 2001 who was in constant pain and on Zoloft, Tylenol #3, Prozac, Clonazepam, Effexor and Soma. From the age of six to 12, SB was active in gymnastics. She had to stop gymnastics when her right hip became painful and, despite lots of therapies and doctors, developed into a constant throbbing pain. Her list of previous therapies to resolve this pain included: physical therapy, prescription medications, deep tissue massage, nerve blocks, acupuncture and Feldenkrais. At the time of her initial consult, she was almost suicidal because the pain was so bad. On physical examination, she had joint hypermobility throughout her body, with a Beighton Hypermobility Score of 6. After a thorough discussion that her prognosis was good but would require a lot of Prolotherapy, she and her mother agreed that SB should start Prolotherapy on her right hip, which was diagnosed as hip joint instability with labral tear.
SB came in somewhat regularly for a two year period, during which time she received dextrose Prolotherapy with sodium morrhuate. She was slowly weaned off of all of her medications. By the time was she was 20, her hip was stable and pain free. She was back to regular exercise and attending college. From the years 2002-2007 she was seen once to twice per year because of joint instability in other areas including the shoulder, neck and elbow. The reason she came to the office in March 2009 was for what she called “tune up treatments” of her right hip and shoulder, at which time she wrote she was forever grateful for Dr. Hauser and the Prolotherapy treatments. She was seen once in 2010 for the same “tune-up treatments.” She noted that the Prolotherapy had gotten her 95% better, but could feel the right hip and neck symptoms recurring.
DISCUSSION:
It is important to note for patients with JHS and EDS that, in some instances, Prolotherapy can give permanent relief to an unstable joint. Sometimes, perhaps because of the genetic component to the conditions, patients with JHS and EDS may need what SB calls “tune-up” treatments once or twice a year. While this is not ideal, the patients typically don’t complain because the rest of their lives are extremely “normal.” Even if a joint becomes too unstable, they have the knowledge that Prolotherapy can always be used. There is comfort in this fact. SB has not taken pain medications, except an occasional acetaminophen, in years. She has been off anti-depressants and anti-anxiety medications for over eight years, and has not seen a psychiatrist in over 10 years. She is one of the most delightful people I have ever had the opportunity to meet and treat.
CASE STUDY: ACTIVE 61 YEAR-OLD FEMALE WITH JHS
In January 2009, BB, a 61 year-old skier, came to Caring Medical saying she “didn’t want anything to slow her down.” BB always knew she had a tremendous amount of joint flexibility, and thus, excelled at yoga as well.
She had a significant past medical history with five years of suffering with bilateral hip, knee, and elbow pain. She continued to be active, including skiing with a very restrictive knee brace, despite her right knee MRI showing a medial meniscus tear, and her right hip MRI showing a high-grade partial-thickness tear involving the gluteus minimus insertion onto the right greater trochanter as the dominant finding with paritendonitis and trochanteric bursitis; low-grade tenoosseous strain of the iliopsoas insertion the lesser trochanter without tendon tear; more substantive iliopsoas bursitis. BB was a strong natural medicine advocate and exclaimed that “No orthopedic surgeon is doing surgery on me!” She was told by a skiing friend to look into Prolotherapy.
BB was diagnosed with JHS and like SB, had evidence of hypermobility throughout. Her Beighton Hypermobility Score was only 4, but many joints had excessive mobility. She was told that she was an excellent Prolotherapy candidate, but because so many joints were involved it would require some time for all of the instability to resolve.
BB was seen at Caring Medical on 10 occasions over the course of the next two years for treatment. Her elbow responded after four treatments, allowing her to get back to exercise, which included weights and push-ups. Her right knee needed five treatments, and her hips each needed nine treatments. Now BB is back to cycling up and down the hills of Colorado and skiing at a high level without braces and without pain.
DISCUSSION:
Some patients with JHS and EDS can function at a high level for most of their lives without needing a lot of medical intervention. In BB’s case, her body didn’t start to suffer the effects of her hypermobility until she was in her mid 50’s. She is an extremely motivated and active person who tried everything she knew to stabilize her joints. When the orthopedic surgeons in Colorado started talking about various “potential” surgeries for her, she looked into Prolotherapy. I suspect that with her extreme sports mentality I may be seeing her periodically for a while. But I am happy for her being able to get back to all of her activities without braces, and look forward to her having an extremely “active” retirement!
CASE STUDY: 48 YEAR-OLD NATIONAL CALIBER ATHLETE WITH PELVIC FLOOR DYSFUNCTION AND JHS
JD came to Caring Medical in extreme distress because she was no longer able to work as a physiotherapist, athletic trainer and Pilates instructor. She was a 48 year-old wife and mother from Ontario, Canada and her pelvic pain had completely disabled her. She explained that her previous life as an athlete included Canadian National rhythmic gymnastics team, international level dragon boat and outrigger paddling, recreational triathlons, cross country skiing and water skiing.
JD always had what she called “extreme flexibility.” She had a series of injuries including the following:
- 2004 – plantar fascia pain
- 2006 – severe hip pain on the greater trochanter
- 2007 – inguinal pain, requiring inguinal hernia repair x 2
- 2008 – right groin exploratory surgery and inguinal nerve ablation. Her right groin pain did not resolve. MRIs at this time revealed a torn rectus abdominus, right hip dysplasia, and labrum tear.
- 2009 – right rectus abdominus repair and removal of mesh. Re-injury of right inguinal area. Another right inguinal hernia repair with mesh.
JD’s first appointment at Caring Medical was in August 2009. She had multiple complaints but her primary pain areas were the pelvic floor, pubis, groin, left knee and left ankle. She received some Prolotherapy in Canada previously, but because she did not feel the technique used was aggressive enough, she was not happy with the results. JD said her main goal was get to back to teaching Pilates full time. The pain was completely disabling her from working and driving, and she was becoming very depressed. Her pain was increased with most movements and activities including sitting, standing and walking. She was diagnosed with JHS with her main problem being subluxation of the pubic symphysis. She was felt to have pubic instability and this was causing the majority of her pelvic pain. She had instability of the left knee and left ankle. These areas were treated with dextrose Prolotherapy with sodium morrhuate every four to six weeks. When JD came for her third visit in December 2009 she noted that she was feeling much better. Her groin pain had improved to the point that she was water jogging two to three times per week and doing some core workouts. She started working again, two mornings per week, and was able to drive short distances. On this third visit, she started treatment on her right hip because of popping, clicking and pain from hip joint instability. She was feeling much stronger and less pain overall until she re-injured her right oblique abdominal muscle and this started her right pubic/groin pain again.
At her February 2010 visit, the pubic symphysis was treated again, as well as the right hip. At this visit, JD noted a new pain in her lower right back which was also treated with dextrose Prolotherapy with sodium morrhuate at that time. Over the course of the next year, JD was seen in the office three times (including seven months between two of the visits) necessitating treatment to her left knee, right hip, and new-onset metatarsalgia of her left foot. To date, her disabling groin pain is down to a manageable level, but feels that some of the pain is secondary to the two meshes she has in her. JD is back to work, but not full time like we had hoped.
DISCUSSION:
When writing case studies, it is often difficult to illustrate the extreme disabling effects of JHS and EDS. I included the case of JD to show that a national caliber athlete can be broken down by these conditions to the point where she could not even work as a full-time athletic trainer/Pilates instructor. In her case, she was on the verge of a nervous breakdown prior to Prolotherapy, and shed many tears at her first consultation. When she was most recently seen, in February 2011, it was primarily because she had fallen on the ice and re-aggravated her right hip and left knee pain. Her groin was not treated, which was the original disabling injury for which she first came to Caring Medical. JD no longer suffers anxiety about when her next joint is going to sublux, because she knows she can get Prolotherapy to treat future injuries. The peace of mind that comes with Prolotherapy for JHS and EDS patients goes a long way.
CONCLUSION
Joint Hypermobility Syndrome (JHS) and Ehlers-Danlos Syndrome are both heritable disorders of connective tissue (HDCT) characterized by joint laxity and hypermobility. The conditions are both genetic disorders of collagen synthesis, where the adverse effects of tissue laxity and fragility can give rise to clinical consequences that resonate far beyond the confines of the musculoskeletal system. Both conditions have as their hallmark generalized hypermobility which can affect almost every bodily system. The hypermobility can be documented by the Brighton criteria which involves the objective measurement of the hyperextensibility of various joints. While the major presenting complaint of JHS and EDS is arthralgia in multiple joints, if the hypermobility is left unchecked, joint dislocations and degeneration may prevail. While traditional medical treatments, including education and lifestyle advice, behavior modification, physiotherapy, taping and bracing, exercise prescription, functional rehabilitation and pain medications offer some symptomatic control, they do little in regard to curbing the progressive debilitating nature of the diseases. The excessive joint mobility, with its subsequent joint degeneration and multiple joint dislocations, can then lead the individual to seek out surgical intervention, which has suboptimal results in the hypermobile patient population versus the normal population. As such, some patients with JHS and EHS are seeking alternative treatments for their pain including Prolotherapy.
Prolotherapy offers great hope for those with symptoms from generalized hypermobility because it is designed to successfully treat the ligament and tissue laxity that accompanies JHS and EDS. Some of the rationale for using Prolotherapy for patients with EDS and JHS are that it has a high safety record, is comprehensive (all or most joints can be treated at each visit), is an outpatient procedure, is cost effective (compared to surgery), pain relief is often quick, and it provides joint stabilization. Perhaps its greatest asset is the fact that this one treatment modality can handle most of the painful musculoskeletal conditions that occur in individuals with EDS and JHS. Prolotherapy could also contribute to the treatment of hypermobility disorders also by preventing the development of precocious osteoarthritis. It has long been known that individuals with JHS and EDS suffer with premature osteoarthritis in various joints and the amount of degeneration correlates with the extent of the individuals hypermobility. The combination of extreme hypermobility and repeated injury is presumed to be what leads to the early osteoarthritis. This is most likely the reason that the hypermobility type of Ehlers-Danlos Syndrome is the most debilitating form with respect to musculoskeletal function.
While the primary author has twenty years experience treating JHS and EDS musculoskeletal symptoms with Prolotherapy, future studies will need to be conducted to best document the exact role Prolotherapy has in the treatment of the musculoskeletal symptoms and hypermobility of JHS and EDS and if it can prevent future joint degeneration in these individuals.
BIBLIOGRAPHY
- Grahme R. Joint hypermobility syndrome pain. Current Pain Headache Rep. 2009;13:427-433.
- Grahame R. Joint hypermobility and genetic collagen disorders: are they related? Archives Dis Child. 1999;80:188-192.
- Biro F, et al. The hypermobility syndrome. Pediatrics. 1983;72:701-706.
- Gedalia A, et al. Joint hypermobility in pediatric practice-a review. Journal of Rheumatology. 1993;20:317-374.
- Hollister DW. Heritable disorders of connective tissue: Ehlers-Danlos syndrome. Pediatric Clinics of North America. 1978;25:575-591.
- Callewaert B, et al. Ehlers-Danlos Syndromes and Marfan Syndrome. Best Pract Res Clin Rheumatolol. 2008;22:165-189.
- Bravo JF. Ehlers-Danlos Syndrome, with special emphasis in the joint hypermobility syndrome. Rev Med Chil. 2009;137:1488-1497.
- Yeowell HN, et al. The Ehlers-Danlos Syndromes. Semin Dermatol. 1993;12:229-240.
- Fernandes NF, et al. A “hyperextensive” review of Ehlers-Danlos syndrome. Cutis. 2008;82:242-248.
- Larsson LG, et al. Benefits and disadvantages of joint hypermobility among musicians. New England Journal of Medicine. 1993;329:1079-1082.
- Magnusson SP. Viscoelastic properties and flexibility of the human muscle-tendon unit in benign joint hypermobility syndrome. Journal of Rheumatology. 2001;28:2720-2725.
- Simpson MR. Benign joint hypermobility syndrome: evaluation, diagnosis, and management. Journal of the American Osteopathic Association. 2006;106:531-536.
- Byers PH. Ehlers-Danlos syndrome: recent advances and current understanding of the clinical and genetic heterogeneity. Journal of Invest Dermatol. 1994;103(5 Suppl):47S-52S.
- Voermans NC, et al. Neuromuscular involvement in various types of Ehlers-Danlos syndrome. Annals of Neurology. 2009;65:687-697.
- Pepin M, et al. Clinical and genetic features of Ehlers-Danlos syndrome type IV, the vascular type. New England Journal of Medicine. 2000;342:673-680.
- Beighton P, et al. Articular mobility in an African population. Annals of Rheumatic Diseases. 1973;32:413-418.
- Grahame R. The revised (Brighton 1998) criteria for the diagnosis of benign joint hypermobility syndrome. Journal of Rheumatology. 2000;27:1777-1779.
- Russek LN. Examination and treatment of a patient with hypermobility syndrome. Physical Therapy. 2000;80:386-398.
- Bravo JF, et al. Clinical study of hereditary disorders of connective tissues in a Chilean population: joint hypermobility syndrome and vascular Ehlers-Danlos syndrome. Arthritis and Rheumatism. 2006;54:515-523.
- Davies AN, et al. Joint hypermobility syndrome in childhood. A not so benign multisystem disorder? Rheumatology (Oxford). 2005;44:744-750.
- Engelbert RH, et al. Exercise tolerance in children and adolescents with musculoskeletal pain in joint mobility and joint hypermobility syndrome. Pediatrics. 2006;118:e690-696.
- Bendik EM, et al. Joint hypermobility syndrome: a common clinical disorder associated with migraine in women. Cephalalgia. 2011;Feb 2. [Epub ahead of print]. Available at: http://www.ncbi.nlm.nih.gov/pubmed/21278238.
- Ross J, et al. Joint hypermobility syndrome. British Medical Journal. 2011;342c:c7167. Available at: http://www.bmj.com/content/342/bmj.c7167.full.
- Grahame R, et al. Joint hypermobility syndrome is a highly prevalent in general rheumatology clinics, its occurrence and clinical presentation being gender, age and race-related. Annals of Rheumatic Diseases. 2006;54:515-523.
- Grahame R, et al. British consultant rheumatologists; perceptions about the hypermobility syndrome: a national survey. Rheumatology (Oxford). 2001;40:559-562.
- Pacey V, et al. Generalized joint hypermobility and risk of lower limb joint injury during sport: a systematic review with meta-analysis. American Journal of Sports Medicine. 2010;38:1487-1497.
- Lotz JC, et al. Innervation, inflammation, and hypermobility may characterize pathologic disc degeneration: review of animal model data. Journal of Bone and Joint Surgery Am. 2006;88S:76-82.
- Collinge R, et al. Hypermobility, injury rate and rehabilitation in a professional football squad-a preliminary study. Physical Therapy and Sports. 2009;10:91-96.
- De Coster PJ, et al. Generalized joint hypermobility and temporomandibular disorders: inherited connective tissue disease as a model with maximum expression. Journal of Orofacial Pain. 19:47-54.
- Peyron JG. Clinical features of osteoarthritis, diffuse idiopathic skeletal hyperostosis, and hypermobility syndromes. Current Opinions of Rheumatology. 1991;3:653-661.
- Bravo JF. Ehlers-Danlos syndrome, with special emphasis in the joint hypermobility syndrome. Rev Med Chil. 2009;137:1488-1497.
- Wheaton M, et al. The ligament injury connection to osteoarthritis. Journal of Prolotherapy. 2010;2:294-304.
- Bierma-Zeinstra SM. Risk factors and prognostic factors of hip and knee osteoarthritis. Nature Clinical Practice, Rheumatology. 2007;3:78-85.
- Kirk JA, et al. The hypermobility syndrome-musculoskeletal complaints associated with generalized joint hypermobility. Annals of Rheumatic Diseases. 1967;26:419-425.
- Agnew P. Evaluation of the child with ligament laxity. Clinical Podiatric Medicine and Surgery. 1997;14:117-130.
- Gedalia A, et al. Joint hypermobility in pediatric practice-a review. Journal of Rheumatology. 1993;20:371-374.
- Toker S, et al. Presentation of two cases with hypermobility syndrome and review of the related literature. European Journal of Rehabilitation Medicine. 2010;46:89-94.
- Grahame R. What is the jont hypermobility syndrome? JHS from the cradle to the grave. In: Hakim A, Keer R, Grahame R, eds. Hypermobility, Fibromyalgia and Chronic Pain. Elsevier, 2010.
- Byers PH. Ehlers-Danlos syndrome: recent advances and current understanding of the clinical and genetic heterogeneity. J Invest Dermatol. 1994;103(5 Suppl):47S-52S.
- Oderich GS, et al. The spectrum, management and clinical outcome of Ehlers-Danlos syndrome type IV: a 30-year experience. Journal of Vascular Surgery. 2005;42:98-106.
- Callewaert B, et al. Ehlers-Danlos syndromes and Marfan syndrome. Best Pract Res Clin Rheumatol. 2008;22:165-189.
- Savasta S, et al. Ehlers-Danlos syndrome and neurological features: a review. Childs Nerv Syst. 2010: August 10 epub PMID: 20697718. Available at: http://www.ncbi.nlm.nih.gov/pubmed/20697718.
- Voermans NC, et al. Neuromuscular involvement in various types of Ehlers-Danlos syndrome. Annals of Neurology. 2009;65:687-697.
- Voermans NC, et al. Pain in Ehlers-Danlos syndrome is common, severe, and associated with functional impairment. Journal of Pain and Symptom Management. 2010;40:370-378.
- Sacheti A, et al. Chronic pain is a manifestation of the Ehlers-Danlos syndrome. Journal of Pain and Symptom Management. 1997;14:88-93.
- Rombaut L, et al. Musculoskeletal complaints, physical activity and health-related quality of life among patients with the Ehlers-Danlos syndrome hypermobility type. Disabil Rehabil. 2010;32:1339-1345.
- Stanitski DF, et al. Orthopaedic manifestations of Ehlers-Danlos syndrome. Clin Orthop Relat Res. 2000;376:213-221.
- Childs SG. Musculoskeletal manifestations of Ehlers-Danlos syndrome. Orthopedic Nursing. 2010;29:133-139.
- Keer R, et al. Joint protection and physical rehabilitation of the adult with hypermobility syndrome. Current Opinions in Rheumatology. 2011;Mar:23(2):131-136. Available at: http://www.ncbi.nlm.nih.gov/pubmed/21252682.
- Simmonds JV, et al. Hypermobility and the hypermobility syndrome, part 2: assessment and management of hypermobility syndrome: illustrated via case studies. Manual Therapy. 2008;13:e1-11.
- Remvig L, et al. Epidemiology of general joint hypermobility and basis for the proposed criteria for benign joint hypermobility syndrome: review of the literature. Journal of Rheumatology. 2007;34:664-665.
- Ferrell WR, et al. Amelioration of symptoms by enhancement of proprioception in patients with joint hypermobility syndrome. Arthritis and Rheumatism. 2004;50:3323-3328.
- McCormack M, et al. Joint laxity and the benign joint hypermobility syndrome in student and professional ballet dancers. Journal of Rheumatology. 2004;31:173-178.
- Schroeder EL, et al. Ehlers-Danlos syndrome in athletes. Current Sports Medicine Rep. 2006;5:327-334.
- Colloca CJ, et al. Chiropractic management of Ehlers-Danlos syndrome: a report of two cases. Journal of Manipulative Physiol Ther. 2003;26:448-459.
- Fiechtner JJ, et al. Manual and manipulation techniques for rheumatic disease. Med Clin North Am. 2002;86:91-103.
- Hauser RA. The acceleration of articular cartilage degeneration in osteoarthritis by nonsteroidal anti-inflammatory drugs. Journal of Prolotherapy. 2010;2:305-322.
- Palmoski MJ. Relationship between matrix proteoglycan content and the effects of salicylate and indomethacin on articular cartilage. Arthritis and Rheumatism. 1983;26:528-531.
- Rashad S. Effect of non-steroidal anti-inflammatory drugs on the course of osteoarthritis. Lancet. 1989;2:519-522.
- Jerjes W, et al. TMJ arthroscopy in patients with Ehlers-Danlos syndrome: case series. Oral Surg Oral Med oral Pathol Oral Radiol Endod. 2010;110:e12-20.
- Jasiewicz B, et al. Spine deformities in patients with Ehlers-Danlos syndrome, type IV – late results of surgical treatment. Scoliosis; 2010:Nov 25:5:26 from PMID:21108838. Available at: http://www.ncbi.nlm.nih.gov/pubmed/21108838.
- Yen JL, et al. Clinical features of Ehlers-Danlos syndrome. J Formos Med Assoc. 2006;105:475-480.
- Aldrige JM, et al. Thermal capsulorraphy of bilateral glenohumeral joints in a pediatric patient with Ehlers-Danlos syndrome. Arthroscopy. 2003;19:E41. (Pubmed 12724665)
- Rose PS, et al. Total knee arthroplasty in Ehlers-Danlos syndrome. Journal of Arthroplasty. 2004;19:190-196.
- Grahame R. What is the jont hypermobility syndrome? JHS from the cradle to the grave. In: Hakim A, Keer R, Grahame R, eds. Hypermobility, Fibromyalgia and Chronic Pain. Elsevier, 2010.
- Levy HP. Ehlers-Danlos Syndrome, Hypermobility Type. From Pagon RA, Bird TC, Dolan CR editors Gene Reviews (Internet). Seattle (WA): University of Washington, latest revision December 14, 2010. Available at: http://www.ncbi.nlm.nih.gov/books/NBK1279/.
- Reeves KD. Randomized prospective double-blind placebo-controlled study of dextrose Prolotherapy for knee osteoarthritis with or without ACL laxity. Alt Ther Health Med. 2000;6:68-74,77-80.
- Dagenais S. Evidence-informed managed chronic low back with Prolotherapy. The Spine Journal. 2008;8:203-212.
- Fullerton BD. High-resolution ultrasound and magnetic resonance imaging to document tissue repair after Prolotherapy. Archives of Physical Medicine and Rehabilitation. 2008;89:377-385.
- Fullerton BD, et al. Ultrasonography in regenerative injection (Prolotherapy) using dextrose, platelet-rich plasma, and other irritants. Physical Medicine and Rehabilitation Clinics of North America. 2010;21:585-605.
- Liu Y. An in situ study of the influence of a sclerosing solution in rabbit medial collateral ligaments and its junction strength. Connective Tissue Research. 1983;2:94-102.
- Centeno CJ, et al. Fluroroscopically guided cervical Prolotherapy for instability with blinded pre and post radiographic reading. Pain Physician. 2005;8:67-72.
- Hackett G. Referral pain and sciatica in low back diagnosis. Journal of the American Medical Association. 1957;163:183-188.
- Hackett G. Prolotherapy for headache. Headache. 1962;April:3-11.
- Hackett G. Referred pain from low back ligament disability. AMA Archives of Surgery. 1956;73:878-883.
- Hackett G. Ligament and Tendon Relaxation Treatment by Prolotherapy. Fifth Edition. Beulah Land Press, Oak Park, 2000.
- Hackett G. Joint stabilization: an experimental, histologic study with comments on the clinical application in ligament proliferation. American Journal of Surgery. 1955;89:968-973.
- Hackett G. Back pain following trauma and disease – Prolotherapy. Military Medicine. 1961;July:517-525.
- Hackett G. Prolotherapy in whiplash and low back pain. Postgraduate Medicine. 1960;February:214-219.
- Hauser RA, et al. Prolo Your Pain Away! Third Edition, Beulah Land Press, Oak Park, 2008.
- Rabago D, et al. Prolotherapy in primary care practice. Primary Care. 2010;37:65-80.
- Hauser RA, et al. A retrospective study on dextrose Prolotherapy for unresolved knee pain at an outpatient charity clinic in rural Illinois. Journal of Prolotherapy. 2009;2:76-88.
- Hauser RA, et al. Prolotherapy: dextrose Prolotherapy for unresolved neck pain. Practical Pain Management. 2007;7:56-69.
- Hauser RA, et al. Prolotherapy as an alternative to surgery – a prospective pilot study of 34 patients from a private medical practice. Journal of Prolotherapy. 2010;2:272-281.
- Hauser RA, et al. Dextrose prolotherapy for unresolved low back pain: a retrospective case series study. Journal of Prolotherapy. 2009;3:145-155.
- Brown A, et al. Familial precocious polyarticular osteoarthrosis of chondrodysplastic type. New Zealand Medical Journal. 1966;65:449-453.
- Kirk J, et al. The Hypermobility Syndrome-musculoskeletal complaints associated with generalized joint hypermobility. Annals of Rheumatic Diseases. 1967;26:419-425.
- Beighton P, et al. Orthopaedic aspects of the Ehlers-Danlos syndrome. The Journal of Bone and Joint Surgery. 1969;51B:444-453.
- Stanitski DF, et al. Orthopaedic manifestations of Ehlers-Danlos syndrome. Clin Orthop Relat Res. 2000;376:213-221.

